Estimated Read Time: 6–8 minutes
Blog Summary: Dry eye disease can sometimes persist even when standard medications appear to improve the ocular surface. In some patients, ongoing discomfort may be linked to neuropathic dry eye, a form of dry eye associated with altered nerve signaling rather than tear deficiency alone. As understanding of nerve-related ocular pain evolves, clinicians are exploring therapies that target these pathways. One medication being discussed in this context is gabapentin, traditionally used for neuropathic pain. This article explores the relationship between gabapentin and dry eye disease, emerging research on topical formulations, and how compounded ophthalmic gabapentin may support individualized care when symptoms remain difficult to manage
Dry eye disease is one of the most common eye conditions affecting adults today, impacting millions of Americans each year.
American Academy of Ophthalmology (AAO)
The AAO reports:
- 16 million Americans have diagnosed dry eye
- Millions more experience symptoms but remain undiagnosed
It occurs when the eyes do not produce enough tears or when the tears evaporate too quickly or fail to function properly, leaving the surface of the eye inadequately lubricated. This disruption in the tear film can lead to uncomfortable symptoms including burning, stinging, redness, light sensitivity, blurry vision, and the persistent sensation that something is in the eye.
While dry eye can affect anyone, it is more commonly seen in individuals over the age of 50, women, contact lens wearers, and patients with certain autoimmune conditions such as lupus or Sjögren syndrome.
Source: American Journal of Ophthalmology
For many patients, traditional dry eye medications focus on improving tear production, reducing inflammation, or protecting the ocular surface. Over-the-counter artificial tears, prescription medications like cyclosporine or lifitegrast, lifestyle adjustments, and procedures such as punctal plugs are commonly used approaches.
However, not all symptoms originate solely from tear deficiency or inflammation. In some cases, the discomfort patients experience may stem from neuropathic dry eye, a condition in which nerve dysfunction or hypersensitivity contributes to ongoing eye pain and irritation even when the ocular surface appears relatively normal.
Experts in ophthalmology increasingly recognize neuropathic dry eye as a complex form of dry eye disease that may require a different therapeutic approach. Because nerve signaling and pain pathways play a role, certain medications traditionally used for neuropathic pain — such as gabapentin — are being explored as potential options to help manage these symptoms. Compounded formulations may allow healthcare providers to tailor strategies based on a patient’s specific needs.
Let’s explore the relationship between gabapentin and neuropathic dry eye, how nerve-related eye pain differs from traditional dry eye disease, and how compounded medications may offer additional options for patients whose symptoms persist despite standard therapies.
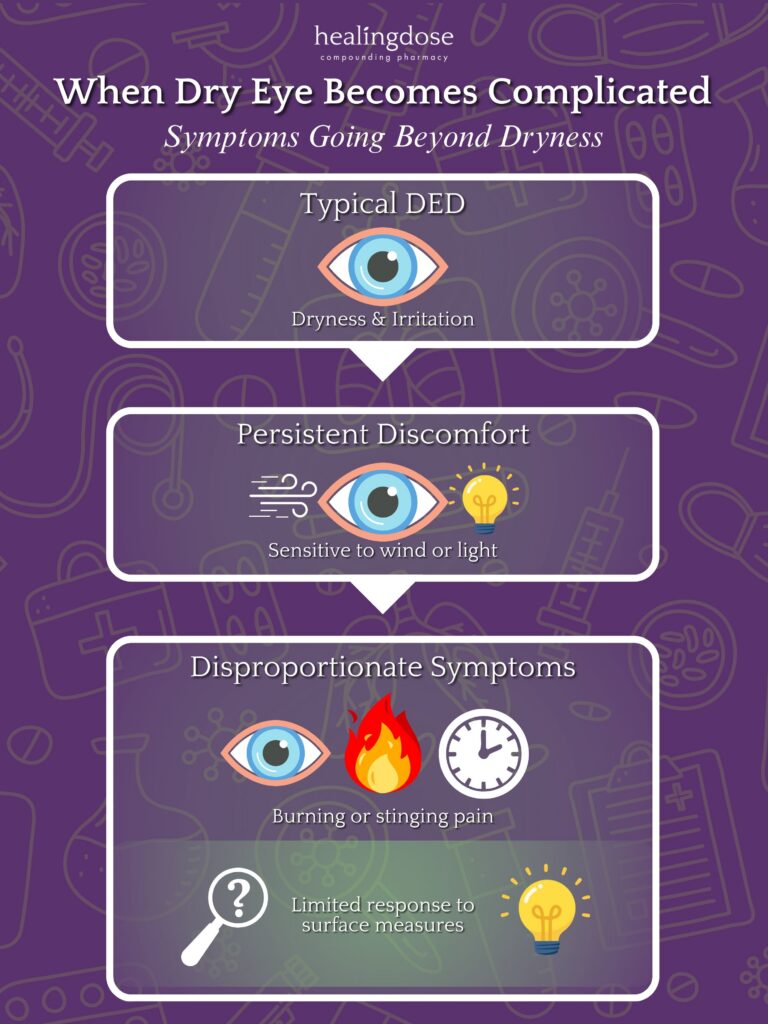
Why Some Dry Eye Symptoms Persist
One of the more challenging aspects of dry eye disease is that symptoms do not always match what appears during an eye exam.
Some individuals may report significant discomfort even when ocular surface findings appear relatively mild. Others may experience fluctuating symptoms that seem to occur without a clear environmental trigger.
Examples may include:
- Persistent burning or stinging sensations
- Discomfort that increases later in the day
- Sensitivity to airflow, light, or wind
- Limited improvement despite regular surface care
These patterns do not indicate patient failure or poor adherence. Instead, they reflect the complex and evolving nature of dry eye disease, which may involve multiple overlapping mechanisms.

Understanding Neuropathic Dry Eye
Dry eye disease is increasingly understood as a multifactorial condition. While tear film instability and inflammation play an important role, research has also highlighted the role of ocular nerve signaling in certain patients.
In some cases, the nerves responsible for sensing and transmitting signals from the eye surface may become more sensitive over time. This heightened signaling may amplify sensations such as burning, irritation, or discomfort.
This phenomenon is often described in research literature as neuropathic ocular pain or neuropathic dry eye.

When clinicians suspect this mechanism may be contributing to symptoms, care discussions may shift beyond tear support alone toward understanding how sensory signaling influences the patient’s experience.
If dry eye discomfort continues despite regular care, discussing symptom patterns with your eye doctor may help guide next steps. In some cases, physicians may evaluate whether nerve-related mechanisms are contributing and whether individualized options, including compounded medications, should be considered.
The Relationship Between Gabapentin and Dry Eyes
Within discussions of neuropathic dry eye, physicians may explore medications known to influence nerve signaling. One medication that often appears in these conversations is gabapentin. It is commonly used when neuropathic ocular pain persists despite topical therapy.
Often combined with:
- artificial tears
- cyclosporine
- anti-inflammatory eye drops
Gabapentin is widely known for its role in managing certain types of nerve-related pain in other parts of the body. Its mechanism involves interaction with calcium channels that influence nerve signaling.
In the context of persistent ocular discomfort, this mechanism has led researchers to explore potential connections between gabapentin and dry eyes, particularly in situations where nerve-related signaling may contribute to symptoms.
What Research Says About Gabapentin & Dry Eye Disease
Response to Gabapentin in Neuropathic Ocular Pain Associated with Dry Eye
Published in Investigative Ophthalmology & Visual Science, researchers wanted to better understand why dry eye develops in the context of type 1 diabetes. They explored whether blocking specific regulatory pathways at the ocular surface could influence those changes.
JOURNAL OF CLINICAL MEDICINE
A 2020 study published in the Journal of Clinical Medicine investigated the effects of oral gabapentin in patients with dry eye disease accompanied by neuropathic ocular pain (NOP) — a type of eye pain caused by nerve dysfunction rather than surface irritation alone. The study reviewed 35 patients with chronic dry eye symptoms and neuropathic pain features that had not improved with standard topical medications such as lubricating eye drops.
After initial topical therapy, some patients received add-on oral gabapentin. Researchers found that a subset of patients experienced significant reductions in ocular pain severity and improvements in quality of life, as measured by the Ocular Pain Assessment Survey (OPAS). Patients who responded to gabapentin also showed improvements in non-ocular pain symptoms and overall daily functioning.
The study also observed that patients with systemic comorbidities such as rheumatologic, neurologic, or psychological conditions were more likely to respond to gabapentin therapy. Overall, the researchers concluded that gabapentin may be a beneficial option for dry eye patients with neuropathic ocular pain that does not respond to conventional topical therapies, particularly when nerve-related pain mechanisms are suspected.
Yoon HJ, Kim J, Yoon KC. Treatment Response to Gabapentin in Neuropathic Ocular Pain Associated with Dry Eye. Journal of Clinical Medicine. 2020;9(11):3765. Link
Molecular Mechanisms and Therapeutic Potential of Gabapentin with a Focus on Topical Formulations to Address Ocular Surface Diseases

PHARMACEUTICALS
A 2024 review highlighted the emerging potential of topical gabapentin eye drops as a novel approach for managing ocular surface diseases, particularly when pain is a major component. Unlike oral gabapentin, which has been studied for systemic neuropathic pain control, topical formulations are being explored as a way to deliver gabapentin directly to the eye while potentially limiting systemic side effects.
The review describes preclinical research suggesting that gabapentin eye drops may offer several benefits at the ocular surface, including analgesic, anti-inflammatory, and tear-supporting effects.
In experimental models, topical gabapentin reduced signs of ocular inflammation, improved discomfort, and appeared to support tear production rather than suppress it. The article also discusses evidence that gabapentin may help protect the ocular surface by improving tear film stability, corneal epithelial healing, and corneal nerve health.
Importantly, the review notes that gabapentin eye drops do not appear to act like a topical anesthetic, meaning they may help reduce pain without impairing corneal sensation or decreasing tear secretion. This distinction makes topical gabapentin particularly interesting for conditions such as dry eye disease, neuropathic ocular pain, corneal ulcers, and other painful ocular surface disorders.
Overall, the article presents gabapentin eye drops as a promising investigational and compounded option in ocular surface care. However, much of the evidence discussed is still preclinical or early-stage, and more human clinical research is needed to better define their role in dry eye and neuropathic ocular pain therapy.
Rusciano, D. (2024). Molecular mechanisms and therapeutic potential of gabapentin with a focus on topical formulations to treat ocular surface diseases. Pharmaceuticals, 17(5), 623. Link
When Might Gabapentin Be Considered in Dry Eye Management?
Every patient’s experience with dry eye disease is unique. When symptoms persist despite conventional care, physicians may evaluate whether multiple mechanisms are contributing to discomfort.
The following hypothetical scenarios illustrate situations in which discussions around gabapentin and dry eyes may arise within provider-guided care.
Symptom–Sign Mismatch: When Discomfort Exceeds Surface Findings
In some cases, ocular surface findings appear relatively mild, yet the individual reports persistent burning sensations that worsen later in the day.
Artificial tears may offer limited alignment with symptom severity. In these situations, the ophthalmologist may evaluate whether nerve-related signaling could be contributing to the patient’s experience and may discuss whether compounded options could be appropriate as part of a broader care conversation.
Sensory Amplification: When Everyday Stimuli Trigger Discomfort
Some patients describe discomfort triggered by everyday stimuli such as blinking, light exposure, or air movement.
The sensation may feel warm, abrasive, or disproportionate to visible dryness. When symptom patterns suggest heightened sensory signaling, clinicians may discuss potential approaches that address nerve-related mechanisms.
Within these discussions, compounded gabapentin formulations may be discussed within individualized care planning.
Chronic Mixed-Mechanism Presentation: When Surface Disease and Nerve Signaling Overlap
In long-standing dry eye disease, surface changes and nerve-related signaling may interact over time.
A patient with a history of ocular surface dryness may continue experiencing discomfort even as surface therapies improve tear stability. In these situations, physicians may reassess the broader picture of the disease and explore additional options within a personalized care plan.
When used in ophthalmic formulations, gabapentin is typically prepared through compounding and prescribed off-label based on physician evaluation.
Why Compounding May Be Considered in Complex Dry Eye Care
Most commercial eye medications are produced in standardized strengths and fixed dosage forms. While this approach supports some patients, it cannot accommodate every clinical situation.
When symptoms become complex or individualized, clinicians may look for greater formulation flexibility rather than simple escalation of therapy.
Pharmaceutical compounding allows medications to be prepared according to prescriber instructions and patient-specific considerations.
In dry eye care discussions involving gabapentin and dry eyes, compounding may allow physicians to explore customized ophthalmic preparations when appropriate.
At Healing Dose Compounding Pharmacy (HDRx), medications can be prepared based on prescriber instructions and patient-specific considerations. This flexibility may include:
- Customized strengths or ingredient profiles
- Non-sterile formulations when commercial formats are not suitable
- Sterile ophthalmic preparations developed under USP <797> standards
As a PCAB- and ACHC-accredited compounding pharmacy, HDRx supports prescriber-driven personalized care with a focus on quality, consistency, and collaboration.
The Role of a Healing Dose Compounding Pharmacy in Dry Eye Disease
In complex dry eye disease, compounding pharmacies may support clinicians by translating prescriber-guided therapy plans into customized formulations.
Compounding functions as a collaborative step that helps align formulation and delivery with provider intent.
At Healing Dose Compounding Pharmacy (HDRx), we provide practitioners with the resources to streamline prescription management:
- Provider Portal
- Submit/Manage Prescriptions
- Approve Refills
- View Patient History
- Billing Tools
- Ship Medications to Patients
- More!
- Rx Order Forms
- Prescription shipping to Michigan, Ohio, Wisconsin, Minnesota, and Florida
- Nationwide shipping of non-prescription products

For patients experiencing persistent dry eye symptoms, including discomfort sometimes described as neuropathic in nature, Healing Dose pharmacists may help answer general questions about compounding and how these options may be discussed with a healthcare provider.
For prescribers interested in discussing gabapentin formulation considerations, Healing Dose Compounding Pharmacy (HDRx) welcomes collaborative conversations around personalized, provider-guided care.
Frequently Asked Questions About Gabapentin and Dry Eyes
Why might gabapentin be discussed in cases of persistent dry eye discomfort?
Gabapentin is known for influencing nerve signaling pathways involved in certain types of pain. In some clinical discussions, physicians may explore whether nerve-related signaling contributes to persistent dry eye symptoms. When this mechanism is suspected, gabapentin may be discussed as part of a broader care evaluation.
What is neuropathic dry eye?
Neuropathic dry eye refers to situations where ocular discomfort may involve heightened nerve signaling rather than tear film instability alone. Patients may experience burning, sensitivity to airflow, or discomfort that appears stronger than clinical findings suggest.
Are gabapentin eye drops commercially available?
Commercial ophthalmic gabapentin products are not widely available. When topical formulations are discussed, they may require preparation through pharmaceutical compounding based on prescriber guidance.
Why would gabapentin be compounded for dry eye?
Compounding may allow medications to be prepared in customized strengths or dosage forms when commercially manufactured products do not meet the needs of a specific care plan.
References
Betz, J., & Galor, A. (2025). Navigating the Dry Eye Therapeutic Puzzle: A Mechanism-Based Overview of current treatments. Pharmaceuticals, 18(7), 994. Link
Mcmonnies, C. W. (2017). The potential role of neuropathic mechanisms in dry eye syndromes. Journal of optometry, 10(1), 5-13. Link
National Eye Institute. (2025, August 11). Dry Eye | National Eye Institute. Link
Rusciano, D. (2024). Molecular Mechanisms and Therapeutic Potential of Gabapentin with a Focus on Topical Formulations to Treat Ocular Surface Diseases. Pharmaceuticals, 17(5), 623. Link
Schaumberg, D. A., Sullivan, D. A., Buring, J. E., & Dana, M. R. (2003). Prevalence of dry eye syndrome among US women. American journal of ophthalmology, 136(2), 318-326. Link
Thulasi, P., & Djalilian, A. R. (2017). Update in Current Diagnostics and Therapeutics of Dry Eye Disease. Ophthalmology, 124(11), S27–S33. Link
- Yang, C., Anand, A., Huang, C., & Lai, J. (2023). Unveiling the Power of Gabapentin-Loaded Nanoceria with Multiple Therapeutic Capabilities for the Treatment of Dry Eye Disease. ACS Nano, 17(24), 25118–25135. Link