Estimated Read Time: 12–14 minutes
Blog Summary:
This blog explains how menopause-related hormonal changes — especially declining estrogen — can disrupt the vaginal microbiome, leading to symptoms like dryness, irritation, and discomfort. It highlights the role of Lactobacillus and vaginal pH in maintaining balance, and how these systems shift during menopause.
The article walks readers through care pathways, starting with over-the-counter options and progressing to hormone-based approaches such as HRT and bioidentical hormone replacement therapy (BHRT). It emphasizes that responses to therapies vary, and that a more patient-specific approach may be considered when standard therapies do not align with symptom patterns or tolerability.
A strong focus is placed on compounded BHRT as a customizable option, allowing prescribers to tailor hormone combinations, strengths, and delivery methods. Real-world patient scenarios illustrate how symptoms and therapeutic needs differ, reinforcing the importance of personalized therapy.
Key Takeaways for Patients and Providers
- Menopause may disrupt vaginal microbiome balance
- Estrogen decline impacts Lactobacillus and vaginal pH
- Symptoms may include dryness, irritation, and discomfort
- Options range from OTC to hormone-based approaches
- Compounded BHRT allows for patient-specific therapy
Important Note:
This content is for informational purposes only and is not intended as medical advice. Health decisions should always be made in consultation with a qualified healthcare provider. Any mention of compounded medications refers to prescriptions prepared by licensed pharmacies based on individual patient needs. These medications are not FDA-approved for safety, effectiveness, or quality.
The vaginal microbiome plays a critical role in maintaining comfort, moisture, and overall vaginal health — especially during menopause.
Understanding how menopause affects the vaginal microbiome can help guide care decisions — from over-the-counter options to hormone-based approaches like HRT and bioidentical hormone replacement therapy (BHRT).
How Does Menopause Affect the Vaginal Microbiome?
During menopause, declining estrogen levels reduce glycogen in vaginal tissue. This may lower Lactobacillus levels and increase vaginal pH, contributing to dryness, irritation, and microbial imbalance.
These shifts are ongoing. For many women, these changes appear gradually — or sometimes unexpectedly — making symptoms feel inconsistent and harder to manage. As a result, symptoms can feel like moving targets that generic, off-the-shelf creams don’t always fully address.
In some cases, relief may involve addressing the hormonal factors that influence the vaginal microbiome.
Understanding the Vaginal Microbiome During Menopause
Menopause changes more than just your temperature; it shifts your internal chemistry. When estrogen levels drop, they influence your vagina’s microbial environment — the system responsible for helping maintain comfort and balance.
What Is the Vaginal Microbiome and How Does It Change in Menopause?
The vaginal microbiome refers to the community of microorganisms that live within the vaginal environment. Rather than acting as a single entity, it functions as a dynamic, supportive ecosystem that helps maintain balance and comfort.
A balanced microbial environment is typically dominated by Lactobacillus species, which produce lactic acid to help maintain an acidic pH. This acidic environment plays an important role in supporting overall vaginal stability and comfort (Park et al., 2023).
- Maintains acidic pH
- Supports tissue comfort
- Helps stabilize the environment
However, the vaginal microbiome isn’t made up of just one type of bacteria. It includes a broader ecosystem of microorganisms that exists in a delicate balance. When this balance shifts — a state sometimes referred to as dysbiosis — the vaginal environment may become more sensitive or less stable.
“Dysbiosis, altered bacterial colonization associated with disease expression, can occur with a loss of specific health promoting bacteria, altered bacterial diversity, or with an increase in pathogens in the microbiome.”
Source: The Microbiota in Gastrointestinal Pathophysiology
During menopause, hormonal changes can influence this ecosystem. As estrogen levels decline, the conditions that support beneficial bacteria may also change, which can contribute to shifts in the bacterial balance and how the tissue feels on a day-to-day basis.
Because this ecosystem is hormone-dependent, declining estrogen during menopause may alter bacterial composition, reduce acidity, and affect tissue resilience.
How Estrogen and Vaginal pH Change the Vaginal Microbiome in Menopause
Think of estrogen as the “nourishment” that helps keep your vaginal tissues resilient. It supports glycogen — the fuel your beneficial bacteria rely on to thrive. When estrogen drops during menopause, that fuel becomes less available, and Lactobacillus levels may decline while vaginal pH begins to rise (Zeng et al., 2024).
This shift can:
- Reduce protective acidity
- Increase sensitivity of vaginal tissues
- Make the environment more prone to imbalance
Over time, these changes may contribute to thinning tissue, reduced elasticity, and dryness — commonly referred to as vaginal atrophy (Brotman et al., 2013).
Research continues to explore how estrogen levels and microbial balance interact during menopause, with growing evidence highlighting the importance of microbiome stability in vaginal health.
Symptoms of Vaginal Microbiome Imbalance During Menopause
For many women, these biological changes show up as a daily reality. Common symptoms of vaginal microbiome Imbalance in menopause may include:
- Vaginal dryness or stinging
- Irritation or burning
- Increased sensitivity to products
- Discomfort during intimacy (dyspareunia)
Collectively, these symptoms are known as Genitourinary Syndrome of Menopause (GSM) (Portman & Gass, 2014). Beyond the physical discomfort, GSM can affect confidence and overall quality of life. It reflects a deeper internal shift — one that may lead patients and providers to explore more patient-specific approaches to care.
“The onset, severity, and type of GSM symptoms may be associated with changes in vaginal microbiota in perimenopausal and postmenopausal women.”
Source: Frontiers in Cellular and Infection Microbiology
How to Support Vaginal Microbiome Balance During Menopause
Since every woman’s hormonal profile is different, finding balance is rarely a straight line. Care often begins with evaluating underlying factors such as hormone levels, tissue health, and sensitivity to formulations.
- Hormonal patterns over time
- Vaginal tissue response
- Tolerance to specific formulations
For many women, this becomes a conversation with their doctor about which approach best reflects how their body is responding.
Options for Addressing Vaginal Microbiome Changes in Menopause
When seeking relief for vaginal dryness, most women start with over-the-counter moisturizers for surface-level comfort or prescription therapies that may address underlying changes (Faubion et al., 2022).
While many women begin with non-hormonal options, these approaches may not address the underlying hormonal drivers of microbiome imbalance. In these cases, providers may explore hormone-based strategies like Hormone Replacement Therapy (HRT), often used to support hormone levels that shift during menopause. However, when needs are individual, healthcare practitioners may suggest a more personalized route to help ensure the dosage and delivery align with your body’s unique needs, through Bioidentical Hormone Replacement Therapy (BHRT).
Local vs Systemic Hormone Therapy
Understanding how hormone therapy is delivered can help clarify therapy decisions.
Local Therapy
- Targets vaginal tissue directly
- Often used for dryness, irritation, and discomfort
- May involve creams, suppositories, or inserts
Systemic Therapy
- Affects the entire body
- May be considered when broader symptoms like hot flashes or night sweats are present
- May involve oral formulations
| Type | Use Case | Forms |
|---|---|---|
| Local | Vaginal symptoms | Creams, inserts |
| Systemic | Whole-body symptoms | Oral capsules, tablets |
Your provider may recommend one or both approaches depending on your symptoms and goals.
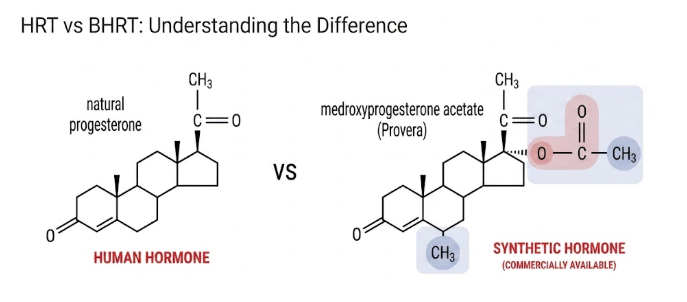
If you are considering hormone therapy, the source and structure of those hormones can play a role in how care is approached. HRT often uses synthetic or animal-derived hormones designed to support changing hormone levels during menopause.
Meanwhile, Bioidentical Hormone Replacement Therapy (BHRT) takes a different approach. These hormones are typically plant-derived and are processed to be structurally similar to those your body naturally produces. Because of this, BHRT is sometimes considered in care plans where more case-by-case clinical decisions are being explored.
- Over-the-Counter: Provides temporary, surface-level moisture but does not address underlying hormonal changes.
- Conventional HRT: Uses standardized formulations, often in preset strengths and delivery methods.
- BHRT: Uses hormones designed to be structurally similar to those naturally produced by the body.
- Compounded BHRT: Allows providers to prescribe customized combinations, strengths, and delivery methods based on individual patient needs and sensitivities.
When Should BHRT be Considered?
In some cases, providers may consider BHRT when standard approaches do not fully address symptoms or are not well tolerated.
- Persistent vaginal dryness despite OTC
- Sensitivity to standard formulations
- Need for customized dosing or delivery
Most care plans begin conservatively. However, if symptoms persist or feel inconsistent, it may be time to revisit your options.
For Prescribers: Clinical Considerations
Evaluate GSM severity and associated microbiome changes
- Assess whether symptoms are localized or systemic
- Consider patient response to prior therapies
- Review sensitivity to excipients or delivery systems
- Determine whether compounded BHRT may support dose or formulation flexibility
Clinical collaboration is important. HDRx partners with prescribers to support hormone therapy plans, including compounded BHRT formulations designed to align with patient-specific dosing, formulation, and delivery preferences.
Compounded medications are prepared by licensed pharmacies based on a healthcare provider’s prescription and are not reviewed or approved by the FDA for safety, effectiveness, or quality. These medications are customized to meet individual patient needs when commercially available options may not be suitable. |
Why Standard Care May Not Work for Every Woman During Menopause
Most therapies are designed with preset strengths and standardized formulas. But menopause doesn’t follow a predictable pattern. As your hormone levels and vaginal bacterial balance shift, your body’s response to a standard dose can vary significantly from someone else’s.
Limitations of Fixed Dosages
When you are limited to predetermined strengths, finding the right balance can feel like a “Goldilocks” problem:
- One dose feels too strong or leads to new irritation
- Another doesn’t provide enough change to feel meaningful
- Adjustments often mean switching to a different product rather than refining the one you’re already using
Sensitivities and Ingredients
Standard medications often contain preservatives, fillers, or stabilizers to support shelf life. For women experiencing increased sensitivity during menopause, these “inactive” ingredients can sometimes contribute to discomfort or localized reactions — making therapy feel just as frustrating as the symptoms.
Usability and Personal Preference
Whether it’s a tablet, a patch, or a cream, your comfort matters. Many women find standard cream bases to be messy, inconvenient, or simply uncomfortable to use consistently. When a therapy is difficult to maintain, consistency can become a challenge.
What to Expect When Starting Hormone-Based Support
Responses to hormone-based approaches can vary.
In many cases:
- Changes may occur gradually
- Adjustments may be needed over time
- Ongoing communication with your provider helps guide care
This process is not immediate — it often evolves based on how your body responds.
Real-World Menopause Scenarios: How Symptoms and Therapy Needs Vary
Menopause symptoms don’t look the same for everyone. That said, the scenarios below demonstrate how those changes can show up — and how different care approaches may be considered along the way.
When Intimacy Feels Like a Hurdle
Maria, 52, noticed that persistent dryness was doing more than causing physical discomfort — it was creating emotional distance in her relationship.
- The Struggle:
She tried various over-the-counter lubricants, but the relief was short-lived and felt “clinical” rather than natural. - The Turning Point:
Her gynecologist recognized that surface-level moisture might not be addressing the underlying hormonal changes influencing the hormonal drivers of her symptoms. - What Her Provider Considered:
They discussed whether a more tailored therapeutic approach — such as compounded BHRT — might better align with her symptoms and overall comfort. - Her Care Plan Included:
A customized BHRT approach, along with follow-up monitoring to evaluate comfort, response, and whether adjustments were needed over time.
When Standard Therapy Feels “Too Much”
Denise, 58, wanted to address her discomfort, but the hormone therapy she was prescribed left her feeling more irritated than expected.
- The Struggle:
Instead of improvement, she experienced localized sensitivity and disrupted sleep. It felt like the standard dose wasn’t aligning well with her system. - The Turning Point:
A hormone specialist explained that responses to hormone therapy can vary, and that formulation, dosage, or even inactive ingredients may influence how the body reacts. - What Her Provider Considered:
They discussed whether a lower-dose or alternative formulation — such as BHRT — might be more appropriate for her sensitivity. - Her Care Plan Included:
An adjusted BHRT plan with changes in strength or formulation, along with ongoing monitoring to refine her care over time.
When “The Usual” Stops Working
Angela, 49, was proactive. At the first sign of dryness, she turned to over-the-counter moisturizers — and initially, they helped.
- The Struggle:
As menopause progressed, those same products no longer felt effective. The dryness returned, along with a new level of sensitivity. - The Turning Point:
Her healthcare provider explained that as hormonal changes continued, shifts in her vaginal microbiome and tissue health might be influencing how her symptoms were evolving. - What Her Provider Considered:
They discussed whether introducing hormone therapy — and potentially adjusting it over time — could better support her changing needs. - Her Care Plan Included:
A tailored approach that included BHRT, with flexibility to adjust formulation or delivery method as her response to care was monitored.
The examples above are illustrative and do not represent guaranteed outcomes. |
How Compounded BHRT Supports Tailored Menopause Care
The relationship between hormones and vaginal microbiome is a two-way street: they constantly influence and respond to one another (Nieto et al., 2025). This is why a one-size-fits-all approach doesn’t always provide consistent results over time. As a woman’s microbiome shifts, hormonal needs may change as well.
When standard, mass-produced therapies don’t align with one’s body’s unique rhythm, a provider may explore more flexible approaches like BHRT. Because of its formulation flexibility, providers can adjust and refine therapy over time based on patient response. How Compounded BHRT Is Prescribed and Prepared
Our pharmacists at HDRx work with practitioners to tailor each woman’s menopause care plan. What can a patient expect?
Step 1: Provider Evaluation
A provider begins by evaluating:
- Symptoms and medical history
- Hormonal patterns
- Sensitivities and preferences
Step 2: Prescription Customization
Based on this evaluation, the prescription may specify:
- Active ingredients (e.g., estrogen, DHEA)
- Adjusted strengths
- Delivery form (cream, capsule, suppository, troche)
- Ingredient inclusions or exclusions
Step 3: Compounding Preparation
Compounding pharmacists then prepare according to the provider’s specifications, with attention to formulation details such as strength, base, and delivery method.

Common Compounded BHRT Formulations for Vaginal Dryness & Menopause Care
At HDRx, we offer women’s health specialists access to a range of compounded BHRT formulation options. Through compounding, prescriptions can be customized to combine active ingredients, remove certain excipients, or adjust dose strengths based on how your provider determines your care plan.
- Estriol:
Often considered in localized formulations, particularly when the focus is on vaginal tissue comfort and hydration. - Estradiol:
A broader-acting estrogen that may be included when both localized and systemic menopausal symptoms are being evaluated. - Combination Estrogens (Bi-Est):
By combining estriol and estradiol, providers may create a formulation that reflects both localized and broader hormone support within a single preparation. - Progesterone:
Commonly included as part of a balanced hormone approach, particularly when estrogen is part of the care plan. It may also be considered in discussions around sleep and overall hormonal regulation. - Testosterone:
Though often associated with men, testosterone also plays a role in women’s health. In some cases, it may be included as part of a broader hormone strategy based on individual presentation. - DHEA:
Sometimes explored in formulations where sexual comfort and tissue support are part of the clinical picture.
These options are compounded in different dosage forms, such as topical creams, oral capsules, troches, and vaginal suppositories.
Who May Benefit From a Patient-Specific Therapy Approach?
Patients that:
- Experience persistent dryness
- Are sensitive to standard products
- Have inconsistent results with current therapy
- Prefer customized delivery methods
BHRT is not appropriate for every patient and should be evaluated by a licensed healthcare provider. |
Michigan Compounding Pharmacy Expertise in Women’s Health and BHRT
Based in Michigan, HDRx works closely with menopause care clinicians and other specialists across the state.
With that foundation, compounding allows a chosen care plan to be adapted in ways that reflect individual patient needs and provider direction.

This may include:
- Different dosage forms, including creams, gels, capsules, troches, and vaginal suppositories, depending on comfort, usability, and clinical intent
- Adjustable strengths, including lower-dose formulations when a more gradual or localized approach is preferred, allowing providers to refine therapy over time
- Combination formulas, such as Bi-est, where multiple hormones are prepared within a single formulation for more streamlined use
- Formulation adjustments, including changes in base or ingredient composition when sensitivity or tolerability is a concern
- Compounding across appropriate preparation environments, with formulations handled under USP-aligned non-sterile or sterile processes depending on prescription requirements
In addition to formulation flexibility, HDRx supports clinicians with streamlined prescription management tools. Through our Provider Portal, easy-to-use RX Forms, or prescribe directly from an EMR for seamless ePrescribing via Surescripts.
HDRx is licensed to ship prescription compounds to Michigan, Florida, Minnesota, Ohio, and Wisconsin, with over-the-counter products available nationwide.
Finding the Right Menopause Care Plan for Your Needs
Menopause is a journey — and it looks different for every woman. Because of that, care isn’t always straightforward. It often reflects personal experiences, shifting symptoms, and changes that don’t follow a predictable path. For many patients, finding the right therapy can feel like a solo mission.
But you don’t have to face this on your own.
For women navigating menopause, speak with your healthcare provider to find out whether compounded BHRT may be appropriate for your care.

For women navigating menopause, speak with your healthcare provider to find out whether compounded BHRT may be appropriate for your care.
For prescribers, contact our team to learn more about customizable hormone therapy strategies, other compounding services, and provider resources.
Frequently Asked Questions About Vaginal Microbiome, Menopause, and Hormone Therapy
What is the vaginal microbiome?
The vaginal microbiome refers to the community of microorganisms — primarily beneficial bacteria like Lactobacillus — that help maintain a balanced vaginal environment. These bacteria support an acidic pH and play a role in maintaining tissue comfort and overall vaginal health.
How does menopause affect the vaginal microbiome?
During menopause, estrogen levels decline, which can reduce glycogen in vaginal tissues. This may lead to lower levels of protective bacteria and an increase in vaginal pH, contributing to symptoms like dryness, irritation, and sensitivity.
How does menopause affect the vaginal microbiome and vaginal pH?
During menopause, declining estrogen reduces glycogen in vaginal tissues. This may lead to lower levels of Lactobacillus and an increase in vaginal pH, which can contribute to dryness, irritation, and microbial imbalance.
How do you restore or fix the vaginal microbiome during menopause?
There isn’t a one-size-fits-all solution. In some cases, providers may recommend moisturizers, lifestyle adjustments, or hormone-based approaches to help support the vaginal environment. The best approach depends on how your body is responding to hormonal changes over time.
What is HRT?
Hormone Replacement Therapy (HRT) refers to medications that are used to support hormone levels — such as estrogen and progesterone — that change during menopause. HRT may be prescribed in different forms depending on a patient’s symptoms and medical history.
What is HRT for women?
For women, HRT is typically used to support symptoms associated with menopause, including hot flashes, night sweats, and vaginal dryness. The specific type, dose, and delivery method are determined by a healthcare provider based on individual needs.
Does HRT cause weight gain?
Weight changes during menopause are common and can be influenced by multiple factors, including hormonal shifts, metabolism, and lifestyle. Some patients may notice changes while on HRT, but responses can vary, and it’s best to discuss concerns with a healthcare provider.
Can estrogen HRT cause acne?
Hormonal changes can sometimes influence skin health, including the potential for acne. Some individuals may experience skin changes when starting or adjusting hormone therapy, depending on how their body responds.
Does HRT help with weight loss?
HRT isn’t typically prescribed for weight loss. However, some patients may notice changes in how their body feels or functions as hormone levels are supported. Outcomes vary, and expectations should be discussed with a provider.
What is compounded BHRT?
Compounded Bioidentical Hormone Replacement Therapy (BHRT) involves customized formulations prepared by a licensed compounding pharmacy based on a healthcare provider’s prescription. These formulations can be adjusted in strength, combination, and delivery method to reflect individual patient needs.
Are compounded BHRT medications FDA-approved?
Compounded medications aren’t reviewed or approved by the U.S. Food and Drug Administration (FDA) for safety, effectiveness, or quality. They are prepared by licensed pharmacies based on a provider’s prescription to meet specific patient needs when commercially available options may not be suitable.
How is compounded BHRT different from standard HRT?
Standard HRT is typically available in fixed doses and formats, while compounded BHRT allows providers to customize hormone combinations, strengths, and delivery methods. This flexibility may be considered when standard options do not fully align with a patient’s needs.
References
- Brotman, R. M., Shardell, M. D., Gajer, P., Fadrosh, D., Chang, K., Silver, M. I., Viscidi, R. P., Burke, A. E., Ravel, J., & Gravitt, P. E. (2013). Association between the vaginal microbiota, menopause status, and signs of vulvovaginal atrophy. Menopause the Journal of the North American Menopause Society, 21(5), 450–458. Link
- Faubion, S. S. M. M. F. N., Crandall, C. J. M. M. M. N. F., Davis, L. D. F. N., Faha, E. K. S. R. P. M., Hodis, H. N., MD, Lobo, R. A., MD, Maki, P. M., PhD, Manson, J. E. M. D. M. N., Pinkerton, J. V. M. F. N., Santoro, N. F., MD, Shifren, J. L. M. N., Shufelt, C. L. M. M. F. N., Thurston, R. C. P. F. F., & Wolfman, W. M. F. F. (2022). The 2022 hormone therapy position statement of The North American Menopause Society. Menopause the Journal of the North American Menopause Society, 29(7), 767–794. Link
- Nieto, M. R., Rus, M. J., Areal-Quecuty, V., Lubián-López, D. M., & Simon-Soro, A. (2025). Menopausal shift on women’s health and microbial niches. Npj Women S Health, 3(1). Link
- Park, M. G., Cho, S., & Oh, M. M. (2023). Menopausal Changes in the Microbiome—A review focused on the genitourinary microbiome. Diagnostics, 13(6), 1193. Link
- Portman, D., & Gass, M. (2014). Genitourinary syndrome of menopause: New terminology for vulvovaginal atrophy from the International Society for the Study of Women’s Sexual Health and The North American Menopause Society. Maturitas, 79(3), 349–354. Link
- Zeng, Q., Shu, H., Pan, H., Zhang, Y., Fan, L., Huang, Y., & Ling, L. (2024). Associations of vaginal microbiota with the onset, severity, and type of symptoms of genitourinary syndrome of menopause in women. Frontiers in Cellular and Infection Microbiology, 14, 1402389. Link